Top Image: Ömer Yıldız/Unsplash
All names have been changed
Keenan, a 38-year-old business owner, is in a hurry. His wife had just suffered a stroke and she needs urgent treatment at Tan Tock Seng Hospital.
Thankfully, when they reached the emergency department on 29 August 2022, she received immediate medical attention. The first few hours are, after all, crucial for a stroke patient.
Keenan recounts the scene. He saw nurses rushing about to answer queries, skilfully shifting their attention between anxious patients and visitors.
Doctors zoom in and out of the emergency department, brows furrowed, their true facial expressions hidden behind, what he imagines, masks steeped with stale air.
When Keenan strains his ear, the hushed and frustrated conversations amongst visitors break up the solemn and sterile atmosphere. Despite the tension, no one dares raise a voice. Everyone understands that healthcare workers are trying their best.
Keenan and his wife would have to wait another 12 hours before being assigned a hospital bed.
Waiting times for admission at Singapore’s public hospitals surged even higher several weeks later. Bed occupancy rates across public hospitals soared, reaching close to full capacity.
Mainstream media reports visitors waiting for as long as 50 hours for admission. The waiting time faced by Keenan and his wife pales in stark comparison.
Healthcare’s Lack of Manpower
A month later, Singapore’s Ministry of Health assured that waiting times for admission have dropped after that 50-hour waiting peak. Minister of Health Mr Ong Ye Kung revealed that Singapore aims to add another 1,900 public hospital beds within the next five years to support swamped emergency departments.
A hospital bed crunch in Singapore’s public hospitals is nothing new. In 2014, Singapore experienced a similar situation. The solution, then? More hospital beds.
Since then, little has changed by way of solving the burgeoning crisis in hospitals across Singapore. According to available data from the Ministry of Health, the number of beds in Singapore’s public hospitals increased year-on-year: From 9,071 beds in 2018 to 9,610 beds in 2020.
Whether a new batch of hospital beds will, once and for all, steer public hospitals away from ever experiencing another crunch remains to be seen.
But, as history suggests, that outcome is unlikely—especially when the COVID-19 virus reinvents itself far too quickly for any medical institution or system to catch up.
And while more hospital beds mean more patients can be attended to at any point, a highly infectious disease (Read: COVID-19 or SARS) could easily create another surge and outstrip the efforts.
Put it this way. It’s like an overcrowded eatery buying more plates to accommodate its customers. Plates are great, but what you also need is more chefs in the kitchen.
Chefs, in this case, are healthcare professionals in the overworked restaurant that is the local public healthcare sector. A manpower crunch seems a perennial problem for the medical community—more beds are merely a band-aid on a gaping wound.
An essential step to solving the lack of doctors in the field is to accept more foreign healthcare workers in our local public hospitals.
Though its objective is clear, the suggestion remains controversial for many locals.

A Fear of The Foreign
Xenophobic sentiments about foreigners stealing local jobs aside are often projected onto the healthcare sector.
A recent tender issued by the Ministry of Health Holdings (MOHH) looking to recruit doctors from India sparked a massive online debate from commentators who quickly jump to conclusions and unapologetically air their concerns.
Misconceptions about foreign doctors, especially those from countries with seemingly less capable medical systems, arise.
The Online Citizen, for instance, was concerned about alleged incidents of fraud in India’s medical education system.
Other concerns included the professional capabilities of potential hires from certain countries—and whether Singapore could look to alternatives, such as attracting Singaporean doctors working overseas to return home.
Ministry of Health Holdings (MOHH) responded via The Straits Times by saying that more than 90 percent of doctors employed by them are local. To the second suggestion, MOHH explains that alternatives, such as attracting overseas Singaporean doctors back to our shores, are already being explored.
“There’s a prejudice about foreign doctors that we should remove from the public,” 25-year-old medical officer Madelyn explains in response to how best to tackle the manpower issue. Madelyn has been a medical officer for two years now. “Just because they’re from another country doesn’t mean they cannot give better or adequate healthcare.”
“I think overseas doctors are very well-trained. Doctors from other countries are much more knowledgeable because of their experience and ability to manage higher patient loads. If they are willing to come over and work, then we should accept them.”
Still, a doctor’s willingness to pack up bags and work in a foreign country does not, in any way, work to quash xenophobic sentiments that foreign healthcare workers are stealing local jobs.
But vacant positions cannot be stolen from a local who was never there in the first place.
The point here is that foreign healthcare workers—doctors, nurses, pharmacists, etc— are essential to a healthy public healthcare sector. Personal politics must be left at the door.

Healthcare Stretched Thin
25-year-old Sherry works in the healthcare sector and was hospitalised on National Day. She waited four days before being allocated to a proper bed—most of her stay was spent on a makeshift trolly bed in a ward.
She admits she didn’t mind it because her condition was not severe. Sherry was eventually moved to a hospital bed on the last day of her stay.
“I think we have enough hospital wards per se. We just don’t have enough manpower to run the wards,” Sherry opines.
“The nurses are either running around attending to queries or tending to a patient. It’s very difficult to get their attention,” she recalls. “They all look very stressed, but I know they are trying their best.” As someone who works in the healthcare sector too, empathy comes easily.
To reduce workloads and eventual stress on our current healthcare workers, Singapore’s medical schools have opened their doors to a larger number of eager-eyed students.
Their combined intake increased by around 60 percent over ten years.
However, this is duly accompanied by an exodus of foreign healthcare workers. Immigration policies have pushed foreign public healthcare workers to leave because of burnout and better working conditions elsewhere.
A recent study published last year by Singapore’s Saw Swee Hock School of Public Health detailed overwork and emotional exhaustion as common causes of burnout among healthcare workers here.
Foreign nurses in Singapore recall more welcoming conditions in countries such as the United States—a stronger currency, more accessible immigration opportunities, and more respect for healthcare workers.
“There were definitely periods when I was a house officer in internal medicine where our resources were stretched very thin,” Madelyn recalls. She tells me that a high patient load is seemingly the rite of passage for all healthcare workers.
“It’s daunting to care for so many patients at one time. Each doctor handles ten to fifteen patients and each patient, especially in internal medicine, has about 15 to 20 issues.”
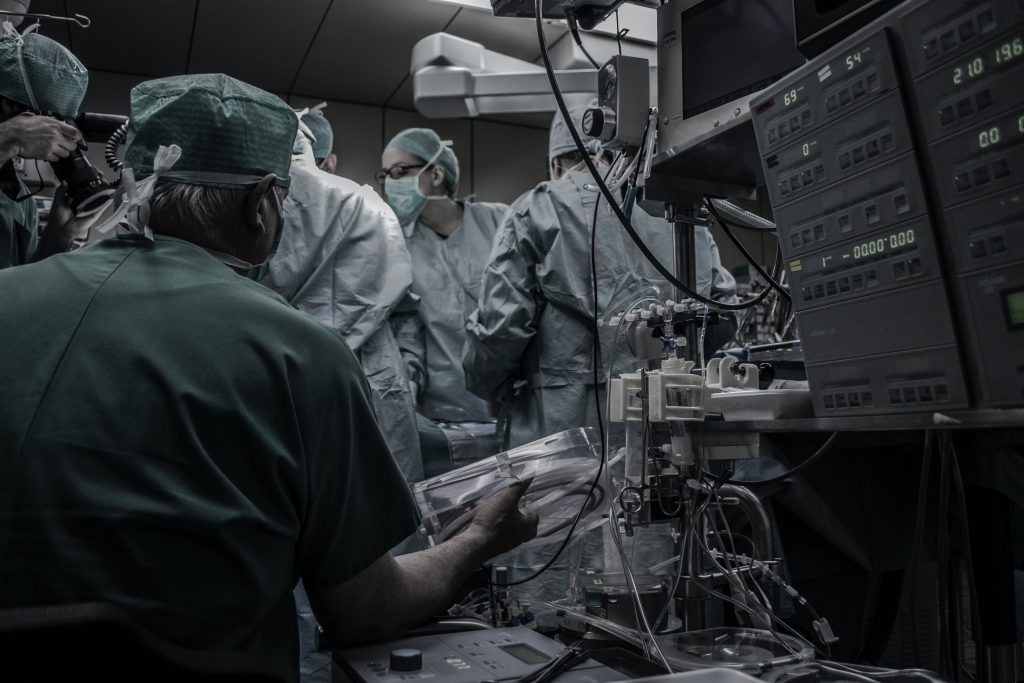
To Discharge or Not To Discharge
Even with more beds and doctors, the long waiting times will not magically disappear from hospitals. Most are unaware of one factor that significantly affects waiting times: Hospital bed turnover rates.
Hospital bed turnover rates are low because discharging a patient goes beyond ensuring a patient is medically fit and capable of going home. That is the baseline. Healthcare workers also have to contend with a patient’s social well-being post-treatment.
“It involves many factors, some of which are intangible,” Madelyn explains. “Whether they’re medically well to go home is one thing. We must also check whether the family is ready to accept them.”
I was surprised to hear her response.
Discharging a patient from a hospital is so closely tied to physical health I had forgotten about the other unseen aspects of patient care.
According to Madelyn, patients could be anxious about their health and request an extra day or two to monitor their condition. Family members must also be equipped enough and ready to help the patient rehabilitate at home.
Junior doctor Yan, who joined the public healthcare sector six months ago, concurs with Madelyn.
“Hospital beds are generally managed by a bed management unit. Doctors place the order, and the rest is up to them. We are always trying to actively discharge people, but there are social aspects we have to take care of.”
“For instance, discharges generally don’t occur at night because it would be difficult for families to pick patients up from the hospital—even if the patient is ready to be discharged. We have to wait until the morning. Naturally, this adds to the waiting times, which we have little control over.”
Yan also begrudgingly admits that increasingly, doctors are more likely to oblige requests for longer stays at hospitals. Part of it is due to fear of lawsuits and allegations of malpractice. The practice of medicine has become more defensive because of it. All it takes is a Karen with a lawyer on speed dial.
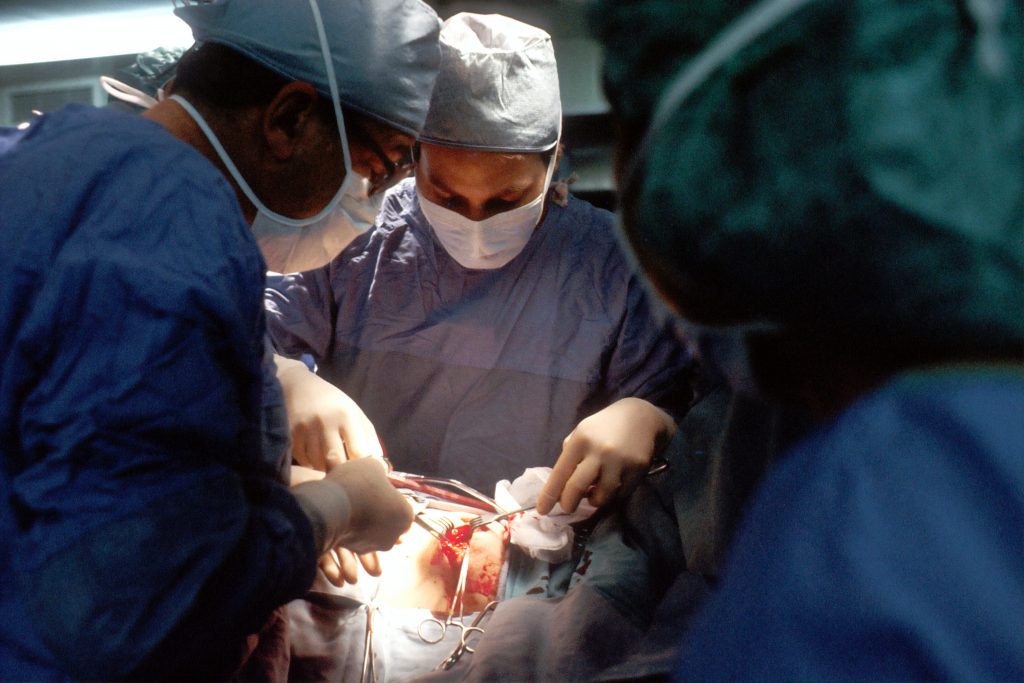
Patience, Please
“Every system at this moment is actually stretched. And we are doing whatever we can to get you the best care,” Yan pleads. “We are doing everything we can, and sometimes we just can’t get you a ward. It’s not because we don’t want to—there just aren’t enough to go around.”
Yan speaks in a slow, measured tone, probably exhausted by the shift he had just completed. During our conversation over a video call, l see nurses and doctors zooming past in the background.
Yan quickly leaves the hospital, unbothered by the flurry of activity behind him. That will have to wait.
“I would strongly suggest visiting your primary care physician if emergency department physicians advise you to do so,” he advises. It is common advice from back before the pandemic of 2020. “There is this misconception that you will receive better care at a hospital. Some conditions can be treated well by family medicine doctors or your GP.”
A shadow of a nearby building casts over Yan as he exits. Streetlamps blur the screen. It’s 9PM—10 hours or so until the start of his next shift.
“I hope patients who come in will understand that when you don’t see us, we are probably doing work. I hope you understand that.”
For Keenan, waiting for updates from healthcare workers when he visited a public hospital was something he could not do. Fortunately, he had the means to seek a second and third opinion in private healthcare.
“We were privileged enough to seek different opinions on my wife’s condition. Of course, you spend more money, but you get a better sense of what’s happening with the treatment plan and can ask more questions.”
“I tried calling for updates when my wife was in public healthcare. But I would either get minimal updates from the doctors or had to call them many times,” Keenan recalls.
Given the seriousness and time-sensitivity of his wife’s condition, Keenan had little choice but to switch to private healthcare, where higher fees meant a more intentional and delicate handling of matters.
Still, for Singaporeans who don’t have such means, public healthcare remains their go-to in times of need.
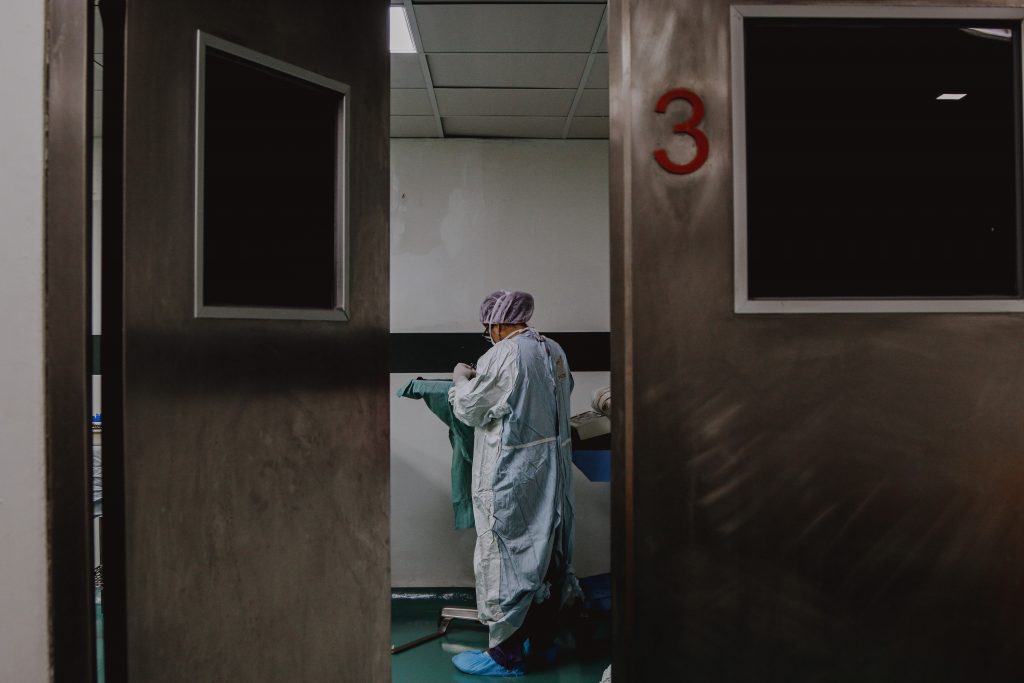
Reciprocating Care
Sufficient hospital beds for Singapore’s entire population is a fever dream. We don’t even have space for new BTO flats. The country might need to reclaim more land to ensure there’s a hospital bed with every Singaporean’s name on it.
A public healthcare sector staffed only with locals is more realistic but is it, really? The fact is that not everyone can or wants to be a doctor. And even if we opened more spots in local medical schools—an arrangement that’s already in place—the public healthcare sector will always be short on staffing.
The solution to all of this is simple, but it’s not one that all Singaporeans can accept. Against a backdrop of anti-foreigner sentiments and a fear of more jobs being taken away from locals during an impending recession, the controversial way out is to attract foreign healthcare professionals to our shores.
For some, reality can be a hard pill to swallow. But what choice does Singapore have? For a small country with only 6 million people, something has to give. The question is, should that be our precious healthcare system?







